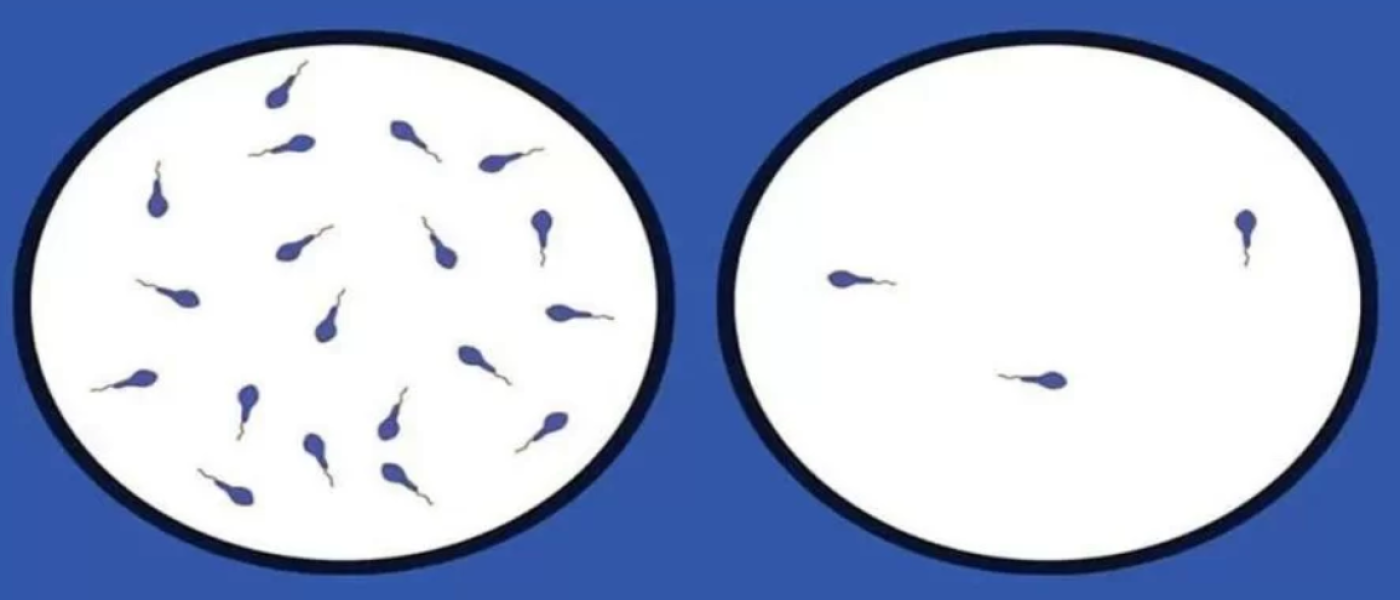
Azoospermia is a major reproductive disorder that causes male infertility in humans. The etiology of this disease is largely unknown. Efforts are on to understand it.
The reliable diagnosis of the absence of spermatozoa in a semen sample is indeed an important criterion not only for diagnosing male infertility but also for ascertaining the success of vasectomy and determining the efficacy of hormonal contraception.
Genetic causes are indeed thought to underlie about half of infertility cases, but also understanding the genetic bases has been a major challenge. Modern genomics tools are empowering more sophisticated exploration of genetic causes of infertility via population-, family-based, and individual studies. Potential therapies are based on genetic diagnostics that are limited until there is certainty about the causality of genetic variants identified in an individual. Genome modulation and editing technologies have, of course, revolutionized the ability to test functionally such variants and also provided a potential means for clinical correction of infertility variants.
The differential diagnosis between obstructive as well as non-obstructive azoospermia is the initial step in the clinical management of azoospermic patients with infertility. It does include a detailed medical history as well as a physical examination, semen analysis, hormonal assessment, genetic tests, and imaging studies. A testicular biopsy is in fact reserved for cases of doubt, mainly in patients whose history, physical examination, and endocrine analysis are inconclusive. The latter does need to be combined with sperm extraction for possible sperm cryopreservation. A detailed analysis of how to make the azoospermia differential diagnosis is essential for understanding the implications of this health issue and its challenges. A coordinated effort that involves reproductive urologists and andrologists, geneticists, pathologists, and also embryologists will indeed offer the best diagnostic path for men with azoospermia.

Azoospermia is indeed broadly classified as obstructive as well as non-obstructive. This differentiation is indeed clinically meaningful, as it does affect patient management and treatment outcomes. Non-obstructive azoospermia (NOA) does relate to an intrinsic testicular defect caused by several conditions that ultimately affect sperm production profoundly.
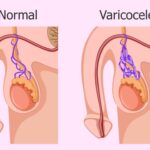
Obstructive azoospermia (OA) does originate from a mechanical block along the reproductive tract, known as the vas deferens, epididymis, or ejaculatory duct. Unlike NOA, spermatogenesis is preserved, and both reconstructive procedures as well as sperm retrieval are typically highly successful in OA patients.
The primary goals of the differential diagnosis are, no doubt, the identification of:
A thorough medical history is essential to help determine the type of azoospermia. It must indeed cover eight critical elements, which are:
The physical exam is indeed very important in the assessment of men presenting with azoospermia. It does start with an appraisal of the person’s overall body characteristics, with a focus on secondary sexual characteristics. Abnormal body hair distribution as well as gynecomastia can be indicative of hypogonadism or hormonal disturbances. Examination of the inguinal and genital areas can reveal scars from previous surgeries that may have injured the testicular blood supply as well as the vas deferens. Other physical defects, like abnormalities of the penis (e.g., hypospadias, epispadias, short frenulum, phimosis, and fibrotic nodules), do need to be evaluated.
A coordinated multidisciplinary effort that entails reproductive urologists and andrologists, reproductive gynecologists, geneticists, and also embryologists is indeed vital to offer infertility patients with azoospermia the best chance of achieving biological parenthood.








©2024. Andro9. All Rights Reserved.